Why Experts Now Say Not to Remove Your Wisdom Teeth? Experts now say you don’t always need to remove wisdom teeth because many remain harmless if they’re healthy, properly aligned, and not causing pain.
In the past, dentists often recommended routine removal to prevent future problems.
Today, research shows unnecessary extraction can lead to complications like infection, nerve damage, or prolonged healing.
Dentists now prefer a “watch and monitor” approach, using regular checkups and X-rays to track changes.
Removal is only advised if there’s crowding, decay, gum disease, or impacted teeth.
This shift helps patients avoid unnecessary surgery while still protecting long-term oral health.
Table of Contents
Quick Table
| Section | Word Count | Key Points |
|---|---|---|
| What Are Wisdom Teeth? | 200 | Evolution, function, third molars |
| Traditional Approach | 200 | Past extraction practices, prophylactic removal |
| Why Experts Say Not to Remove | 200 | Evidence-based dentistry, active monitoring, risks of unnecessary removal |
| What Research Says | 200 | Clinical studies, ADA guidelines, outcomes |
| Risks of Unnecessary Extraction | 200 | Nerve damage, infection, dry socket, cost, recovery time |
| When Removal Is Still Recommended | 200 | Symptomatic teeth, impacted, crowding, pericoronitis |
| Common Myths | 200 | Misconceptions about crowding, aging teeth, prophylactic extraction |
| FAQ | short | 5 questions on symptoms, pain, recovery, costs, timing |
| Conclusion | 200 | Summary, informed decision, evidence-backed recommendations |
What Are Wisdom Teeth?
Wisdom teeth, also known as third molars, are the last set of molars located at the very back of the mouth. Humans typically develop four wisdom teeth, though some people may have fewer or none.
Evolutionarily, these teeth were essential for our ancestors who had larger jaws and relied on a tougher diet of raw plants and meats.
Modern humans, however, have smaller jaws, making wisdom teeth less necessary and often prone to complications.
The function of wisdom teeth has diminished over time due to dietary changes and evolution.
Yet, they still serve as additional chewing surfaces. Most dentists categorize wisdom teeth as either impacted, partially erupted, or fully erupted.
Impacted wisdom teeth are trapped in the jaw or gums and may lead to swelling or infection. Fully erupted teeth may function normally but can pose risks if not monitored.
Understanding the evolutionary context helps explain why not every wisdom tooth requires removal and highlights the importance of evidence-based decisions rather than routine extraction.
Traditional Approach to Wisdom Teeth Removal
Historically, dentists recommended the removal of wisdom teeth as a preventive measure, often during adolescence.
The assumption was that these third molars would inevitably cause dental crowding, pain, or other complications.
This practice, known as prophylactic extraction, became widespread in the 20th century and was considered standard dental care.
Traditional approaches relied heavily on X-rays and dental impressions to predict potential problems.
Dentists often extracted wisdom teeth preemptively, even if patients showed no symptoms. While this method reduced some future complications, it carried inherent risks such as nerve damage, infection, and dry socket.
Despite these risks, prophylactic removal persisted due to routine practices and patient demand.
Modern dentistry has begun questioning this blanket approach. The shift emphasizes individualized treatment based on patient-specific factors like tooth position, jaw size, and overall oral health.
By understanding the traditional mindset, patients can better appreciate why a conservative, evidence-driven approach is now preferred.
Why Experts Now Say Not to Remove Them
Today, many dental experts advocate for a more conservative approach to wisdom teeth management. Rather than removing third molars routinely, the emphasis is on monitoring asymptomatic teeth.
This shift is based on research indicating that unnecessary extractions do not always prevent dental problems and may introduce avoidable complications.
Active surveillance involves regular check-ups, X-rays, and clinical assessments to identify potential issues early.
By monitoring wisdom teeth, dentists can prevent infections, pericoronitis, and other oral health problems without resorting to immediate extraction.
This approach prioritizes patient safety, reduces surgical risks, and aligns with evidence-based dentistry.
Experts highlight that not all wisdom teeth cause problems, and extraction should be reserved for symptomatic cases.
Adopting this strategy ensures that patients receive individualized care, reduces unnecessary costs, and improves overall dental outcomes.
What Research Says
Numerous studies support the conservative management of wisdom teeth.
The American Dental Association (ADA) and other research institutions emphasize that asymptomatic wisdom teeth often do not require extraction.
Clinical trials indicate that routine removal does not significantly reduce the risk of crowding or other dental complications compared to monitoring.
Research also highlights the potential harms of unnecessary extraction. Surgical procedures carry risks such as nerve injury, infection, bleeding, and delayed recovery.
Long-term studies show that many patients with retained wisdom teeth remain symptom-free for decades.
Evidence-based guidelines now encourage dentists to weigh the risks and benefits carefully, focusing on patient-specific factors rather than following outdated protocols.
By relying on research-backed evidence, dental professionals can make informed decisions. This approach ensures optimal patient outcomes and aligns with modern best practices in dentistry.
Risks of Unnecessary Extraction
Removing wisdom teeth when they are not problematic can lead to significant risks.
One of the most common complications is nerve damage, which may cause numbness or tingling in the lips, tongue, or chin. Infections, such as dry socket, are another potential risk, leading to pain and prolonged recovery.
Surgical procedures can also result in bleeding, swelling, and increased healthcare costs.
For younger patients, extraction may disrupt jaw development or increase susceptibility to future dental issues.
Additionally, unnecessary removal can lead to psychological stress and decreased quality of life due to recovery downtime.
Monitoring wisdom teeth reduces these risks. Evidence indicates that keeping asymptomatic teeth under observation is safer and often more cost-effective than preemptive extraction.
Patients can avoid unnecessary complications while maintaining optimal oral health.
When Removal Is Still Recommended
Despite the shift toward conservative management, removal is still necessary in certain cases.
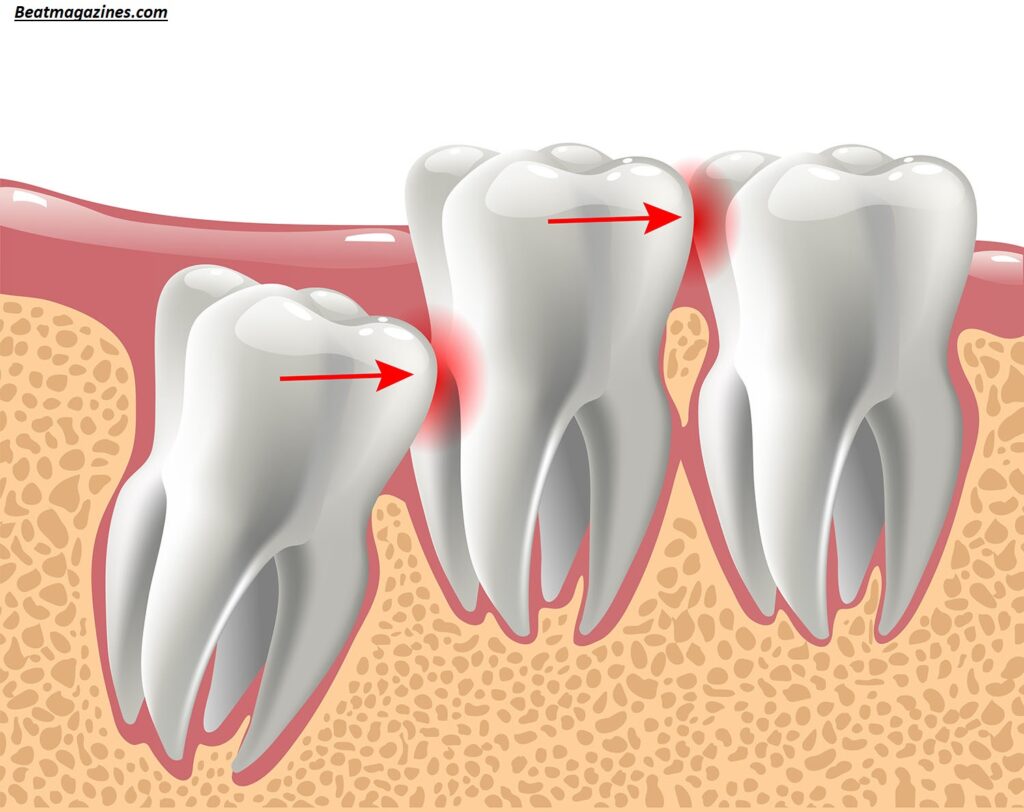
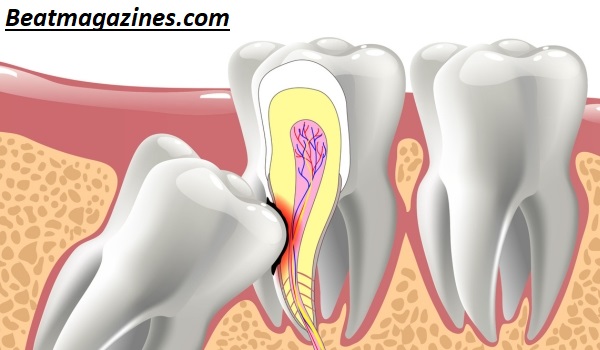
Dentists recommend extraction for symptomatic teeth causing pain, swelling, or infection. Impacted wisdom teeth that press against adjacent teeth may require removal to prevent misalignment or decay.
Other scenarios include repeated pericoronitis, cyst formation, or significant orthodontic concerns. In these cases, the benefits of extraction outweigh potential surgical risks.
Dentists also consider patient age, jaw structure, and overall oral health before deciding on removal.
A tailored approach ensures that extraction is performed only when truly necessary, reducing unnecessary risks and aligning with evidence-based guidelines.
Common Myths About Wisdom Teeth Removal
Many misconceptions surround wisdom teeth management.
A common myth is that all wisdom teeth must be removed to prevent crowding. Research shows that third molars rarely cause significant misalignment in properly monitored patients.
Another misconception is that aging teeth are more likely to become problematic. In reality, asymptomatic wisdom teeth can remain healthy well into adulthood.
Some believe prophylactic extraction guarantees better oral health. However, studies indicate that unnecessary removal can introduce complications without providing significant benefits.
Another myth is that extraction prevents all future dental issues; while it may solve specific problems, it does not replace routine dental care or good oral hygiene practices.
Educating patients about these myths helps promote informed decision-making and reduces the prevalence of unnecessary surgical procedures.
FAQ’s
How do I know if my wisdom teeth need removal?
Dentists recommend removal only if teeth are symptomatic, impacted, or causing infections. Regular monitoring can help detect issues early.
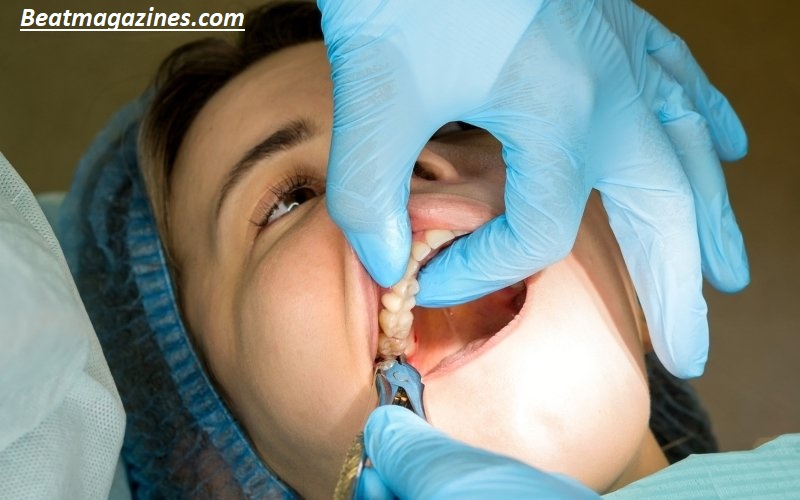
Are wisdom teeth removal surgeries painful?
Most procedures are performed under anesthesia. Post-operative discomfort varies but can include swelling and mild pain, usually manageable with medication.
Can keeping wisdom teeth cause future problems?
Asymptomatic teeth rarely cause issues. Monitoring ensures timely intervention if complications arise.
What are the costs associated with extraction?
Costs vary depending on location, type of extraction, and complexity. Unnecessary removal may lead to avoidable expenses.
How often should I get X-rays for monitoring?
Typically every 1–2 years, or as recommended by your dentist, especially for impacted or partially erupted teeth.
Conclusion
The management of wisdom teeth has evolved significantly.
Evidence now supports that asymptomatic third molars often do not require removal.
By adopting a conservative approach—focused on monitoring, patient-specific assessment, and evidence-based decision-making—patients can avoid unnecessary risks and costs.
Understanding the evolutionary function, potential complications, and scientific research empowers individuals to make informed choices regarding their oral health.
While extraction remains necessary in specific cases, modern dentistry emphasizes balance, safety, and patient-centered care.
Making informed decisions ensures optimal outcomes and aligns with contemporary best practices for maintaining lifelong oral health.
